Tao-Yuan General Hospital, Ministry of Health and Welfare
About us
Products
System architecture diagram
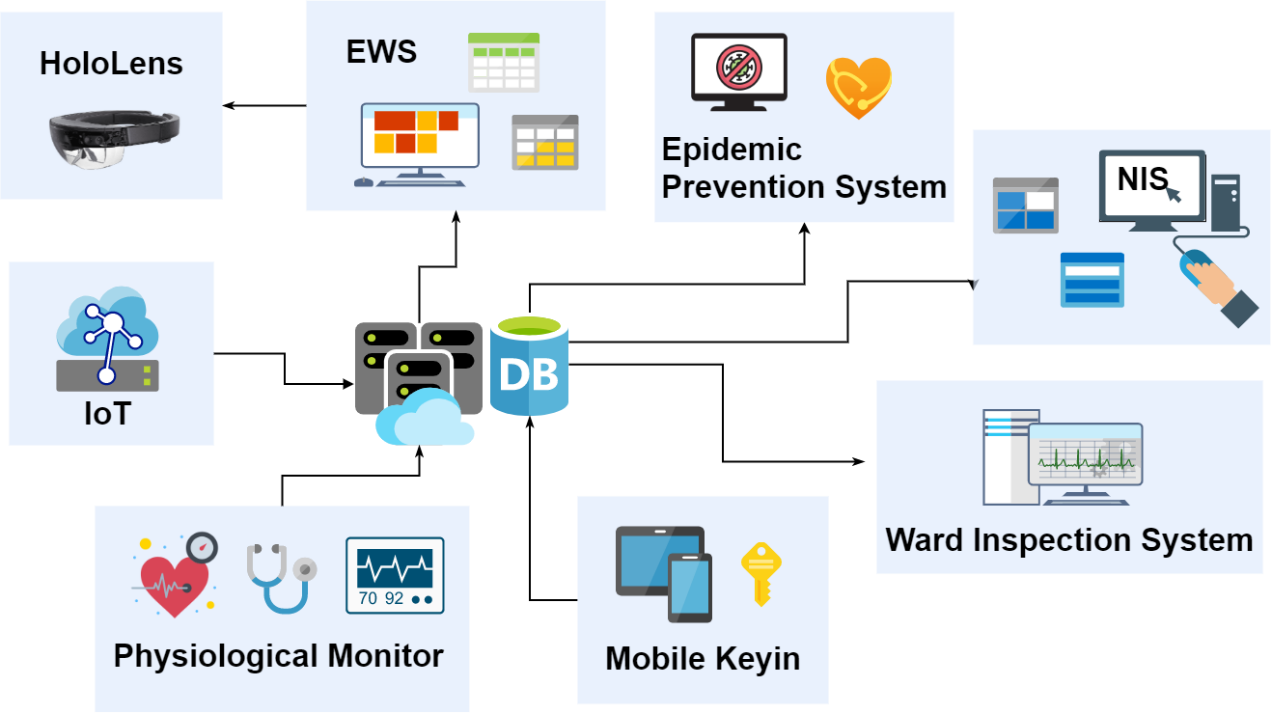
Through the communication network of Taiwan Far EasTone Co., Ltd., upload the data to ASUS Computer Co., Ltd. for cloud computing, and then transfer the calculated data to the database of the hospital's epidemic prevention system for data identification and concatenation of medical data in the hospital. Finally, it interfaces with the EWS system.
In addition to the physiological data routinely measured by medical staff, plus the measurement data of smart watches, the data is presented on the EWS platform in a visual chart for quick identification by medical staff, which not only allows patients to Measure and reduce anxiety, and more effectively reduce the burden on medical staff.
經由台灣遠傳電信股份有限公司之通訊網路,將資料上傳至華碩電腦股份有限公司進行雲端運算,運算後的資料再拋轉至本院防疫系統資料庫,進行資料識別及串接院內醫療資料,最後與EWS 系統介接。除醫護人員例行量測的生理數據外再加上智慧手錶的量測數據,統整以視覺化圖表方式呈現於EWS 平台供醫護人員進行快速識別,不但讓病患隨時都可以透過簡易的自我量測減緩焦躁的情緒,更有效減輕醫護人員負擔。
LINE Login screen
Use LINE to log in to the EWS screen, use the physiological measurement instruments of each ward and the smart watch combined with ASUS Computer's AI and IoT technology applications to measure the physiological data of the case for 24 hours (automatic measurement every 15 minutes, currently only supports systolic blood pressure and pulse), data is updated to the EWS system every 10 minutes.
As soon as the medical team finds an abnormality, it will immediately report it to the LINE group of each department, and the core team will review and decide whether to activate it, establish a network-based team care, and replace the passive reporting and emergency treatment of patients in the past. Effect. In addition, in order to ensure information security, if you want to log in to the system through mobile phones and in-hospital computers, you must enter the exclusive account password of the medical staff, and the patient's personal information will not be displayed on the system screen. All data are identified in the hospital system and integrated with medical information, and then the mobile phone or the computer in the hospital presents a visual chart, so that the medical staff can more accurately observe the trend of the health status of the case and accurately plan the care plan.
使用LINE 登入EWS 的畫面,運用各病房生理量測儀器及結合華碩電腦公司之AI 及IoT 技術應用的智慧手錶24 小時量測個案之生理數據(每15 分鐘自動量測,目前僅支援收縮壓及脈搏),每10 分鐘更新一次數據至EWS 系統,醫療團隊一發現異常則立即通報至各科LINE 群組,由核心小組審核並決定是否啟動,建立網絡式的團隊照護,取代過去被動進行通報及病患急救處置,轉為主動監測數值,達到預警效果。此外,為確保資訊安全,欲透過手機及院內電腦登錄此系統,皆須輸入醫護人員專屬帳號密碼,且病患個資皆不會顯示於系統畫面上。所有數據於院內系統進行識別並整合醫療資料,再由手機或院內電腦呈現視覺畫圖表,使醫護人員能更精確的觀察個案的健康狀況趨勢,準確規劃照護計畫。
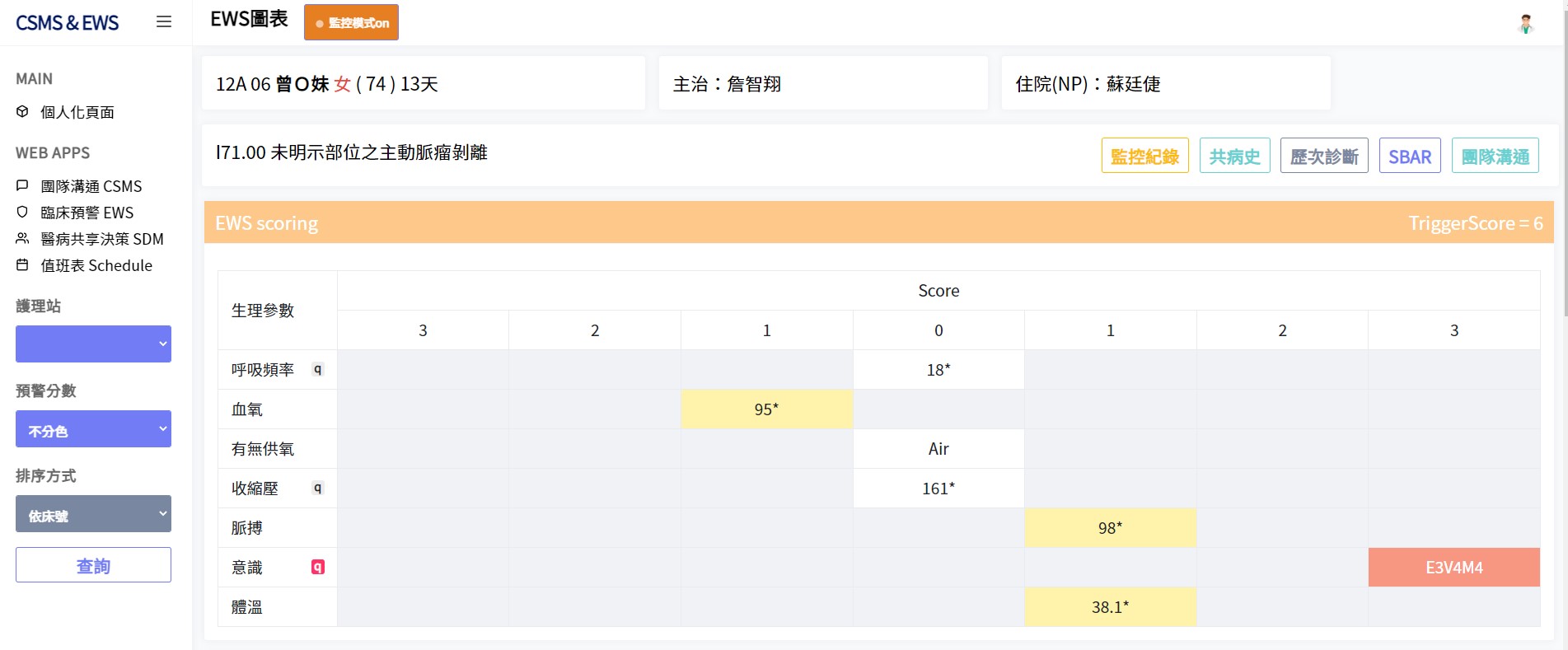
EWS Score
If the patient is female, the gender is shown in red; if the patient is male, it is shown in blue.Convert respiratory rate, blood oxygen, presence or absence of oxygen supply, systolic blood pressure, pulse, consciousness, and body temperature into fractions,Each item is assigned 0 to 3 points, and the total score of 7 points is the patient's score value and the current critical degree of the patient is divided by color.Individual item 0 points are represented in gray, 1 points are represented in yellow, 2 points are represented in orange, and 3 points are represented in red, which are presented on the patient's personal score sheet;A total of 0-3 points for 7 items is shown in gray, a total of 4 points or a single item of 3 points is shown in yellow, a total of 5-6 points is shown in orange, and a total of more than 7 points is shown in red on the nursing station and personal page,The higher the score, the more serious it is. By dividing the score and color, it is convenient for medical staff to quickly identify the current condition of the patient.
病患為女性則性別顯示紅色;男性則顯示藍色。將呼吸頻率、血氧、有無供氧、收縮壓、脈搏、意識、體溫共七項數值區間換算成分數,每項賦值0~3 分,共7 個的總得分為該病患的評分值並以顏色劃分病患當前的危急程度。單項0 分以灰色表示、1 分以黃色表示、2分以橘色表示、3 分以紅色表示呈現於病患個人評分表;7 項加總0~3 分以灰色表示、加總4 分或單項3 分以黃色表示、加總5~6 分以橘色表示、加總7 分以上以紅色表示呈現於護理站及個人化頁面,得分越高表示該項數值越嚴重,藉由分數及顏色劃分,方便醫護人員快速辨識病患當前狀況。
EWS multiple data presentation
The hospital has specially added comorbidity history, past diagnoses, SBAR and team communication functions in the EWS system. In order to make the nursing judgment of medical staff more accurate, the function of co-morbid history and previous diagnosis is added.
The comorbidity history refers to the research announcement data of the Agency for Healthcare Research and Quality (AHRQ) of the United States, and the comorbidity history is automatically analyzed and judged by the arrangement and combination database of thousands of groups of ICD codes imported by the system.
In the previous diagnosis function, the system will automatically bring out all the medical diagnosis of the patient in the past six months and all the medical treatment records of the patient in this hospital from the database of the National Health Insurance Bureau. With these two functions, physicians can provide reference for follow-up diagnosis and treatment.
本院在EWS 系統中特別新增之共病史、歷次診斷、SBAR 及團隊溝通功能。為使醫護人員照護判斷更為精確,加入共病史功能及歷次診斷功能。共病史參考美國健康照護研究與品質局(Agency for Healthcare Research and Quality, AHRQ)研究公告數據,藉由系統匯入的上千組ICD 代碼排列組合資料庫,自動分析判斷並帶入其共病史。而在歷次診斷功能中,系統將自動從健保局資料庫中帶出此病患近半年的所有的就醫診斷,及此病患在本院所有的就診紀錄。藉由這兩項功能,提供醫師後續病情判斷及治療參考。
EWS interface description
By dividing scores and colors, it is convenient for medical staff to quickly identify the current status of patients. The system captures patient vital signs data every 10 minutes, and displays the results on the EWS interface in real time, allowing the medical team to directly view the latest 24 changes in risk scores from the system, not only to grasp the current situation, but also to The risk score grasps the risk of disease deterioration in the next 6 to 12 hours, with warning and reminder functions.
The auxiliary care team provides timely and appropriate medical care immediately, thereby improving patient safety, implementing the concept of precise care, and minimizing preventable emergency incidents and deaths.
藉由分數及顏色劃分,方便醫護人員快速辨識病患當前狀況。透過系統每10分鐘擷取一次病患生命徵象資料,即時將結果彙整顯示在EWS介面,可讓醫護團隊直接從系統上看到最近24次的風險分數變動趨勢,不僅可把握現況,也可以根據風險分數掌握未來6到12小時病況惡化風險度,具有警示及提醒功能,輔助照護團隊即時提供適時適當的醫療照護,進而提升病人安全,落實精準照護理念,將可預防的急救事件及死亡降到最低。
SBAR Shift system
 "SBAR" is a communication method used in shift shifts, which originated from the communication with each other in nuclear submarines, and was later adapted by Kaiser Permanente Hospital to be suitable for health care to improve communication methods. It is an abbreviation for Situation, Background, Assessment, and Recommendation.
"SBAR" is a communication method used in shift shifts, which originated from the communication with each other in nuclear submarines, and was later adapted by Kaiser Permanente Hospital to be suitable for health care to improve communication methods. It is an abbreviation for Situation, Background, Assessment, and Recommendation.
The health status of hospitalized patients can change at any time, so the record of each shift is even more important. The medical staff can use the SBAR function to update the records of the patient's condition and suggestions at the shift of shifts in the morning, noon and evening. to the next healthcare worker in charge.
Using SBAR to achieve the function of "handover management", the use of key shifts not only makes the communication between people or inter-units more efficient and smooth, but also improves everyone's communication skills and medical care quality, thereby reducing Medical Negligence.
「SBAR」為一種運用於交班的溝通方式,源於核子潛艇中彼此的溝通,後被Kaiser Permanente 醫院改編成適用於健康照護,用以改善溝通的方法。其為Situation(狀況)、Background(背景)、Assessment(評估)、Recommendation(建議)之縮寫。住院病患的健康狀況隨時都有可能改變,因此每次交班時的紀錄就更顯重要。醫護人員可透過SBAR功能於每日早中晚交班時更新紀錄病患之狀況及建議等,目的是希望藉由標準化,以清楚、容易明白的方式表達相關訊息,將不必要的細節省略,交接給下一位負責的醫護人員。運用SBAR 達到「交棒式管理」功能,使用重點式交班不僅使人與人或跨單位間之溝通將變得更有效率和更流暢,更可提昇大家之溝通能力及醫療照護品質,進而減少醫療疏失。
The hospital-wide effect of introducing the smart mobile clinical early warning system EWS
The hospital-wide effect of introducing the smart mobile clinical early warning system EWS
Taoyuan is the front line of border epidemic prevention. The Taoyuan Hospital under the Ministry of Health and Welfare shoulders a heavy responsibility. In addition to epidemic prevention medical services, it also provides public medical center-level services in the greater Taoyuan area. In order to improve the service quality of the hospital's medical team, it is the first to use smart medical technology. , to assist the medical team in caring for patients.
During the COVID19 period, he participated in the "Technology Anti-epidemic 2.0" project jointly launched by the State Grid Center of the National Research Institute and Taiwan Zhiyun (TWS) this year, using the cloud intelligent high-speed computing resources of the TWCC platform to improve the Early Warning System (Early Warning System, EWS), reducing the burden on medical staff and improving the quality of emergency care.
Chen Houquan, vice president of the Taoyuan Hospital, said that the hospital's front-line field is very busy. Each medical staff needs to perform a large number of outpatient services and can take care of each patient comprehensively. The challenges faced by the hospital are beyond the imagination of outsiders. Therefore, we actively introduce the auxiliary measures of the clinical early warning system from the British medical system, use big data analysis to extract the substantive content of the data, and use the Line software on the smartphone as the information platform to implement the application of mHealth mobile care (Mobile Health).
The hospital has introduced an intelligent clinical early warning system, based on the patient's physiological measurement information, as an early detection of the patient's condition change (Clinical Deterioration), and immediate allocation of critical resources to reduce patient harm and improve The quality of medical care and the reduction of medical disputes can also effectively manage the clinical medical team and reduce the cost of hospitals. Especially in the era of artificial intelligence (AI) and big data analysis, by downloading the medication history information of the National Health Insurance cloud, the big data analysis of the National Health Insurance database is carried out, and a multiple comorbidity index (Comorbidity Index) is formed as a treatment risk assessment. When the patient's physiological symptoms deteriorate, it can actively and instantly warn, improving the efficiency and accuracy of clinical medical staff.
Based on the patient's multiple comorbidity indicators, an optimized interdisciplinary care team is formed to provide precise care, which not only achieves the best treatment effect, but also avoids potential complications. At present, EWS will take the initiative to identify key patients from patient data, select high-risk patients as the focus of the team, focus medical treatment on high-risk patients, and use the mobile phones of medical staff as a common warning platform to make the data transparent. , and display the warnings and prompts of high-risk patients in different colors on the mobile phone to quickly find out the patient's condition.
Using AI to select high-risk patients, the Ministry of Taoyuan Hospital began to use the team of the Department of Life Sciences of Yangming Jiaotong University to cooperate in development in 2020. With the assistance of TWCC computing resources and the professional service energy of State Grid Center and Taizhiyun (TWS), the entire The system has been developed for more than a year and a half of running-in and testing. It is used to manage 5% of high-risk patients. From the one-hour daily EWS meeting in the hospital when it was first introduced, it has been shortened to the current 10-minute meeting time every day. It is possible to quickly browse and grasp the status of 300 patients, from the past every day. The room rounds were changed to key rounds, which successfully saved manpower time.
With the intervention of EWS, Taoyuan Hospital not only reduces the number of unanticipated first aid cases through the function of real-time warning, but also responds early to speed up the rescue time, thereby improving the mortality rate of the ward after emergency treatment. Through this intelligent solution, the unexpected emergency rate is improved by an average of about 31% every year, and the mortality rate in the post-emergency ward is improved by an average of 50%, saving the precious lives of patients with remarkable results.
At present, the EWS task force in the hospital regularly tracks, discusses and analyzes the use of the system to improve the utilization rate of medical care. It is worth mentioning that some senior medical staff can use professional intuition, such as the physiological characteristics or information of certain patients. , and accurately identify high-risk patients. Chen Houquan believes that this is a very valuable warning mechanism in the future. Through the connection of scientific facts, the accuracy of the early warning system is planned to be strengthened, and the rescue time will be further accelerated.
The introduction of hospital-wide intelligence early warning system (EWS) in medical institutions has become a trend in advanced countries in Europe and North America. In order to enter the era of AI and Big Data smoothly, the Taoyuan General Hospital develops its own intelligent EWS which is capable of providing immediate warning when patients show signs and symptoms of deterioration.
The core systems and technologies of the early clinical warning system are as follow:
1. A Comorbidity Index based on the National Health Insurance MediCloud System.
2. An Early Warning System based on physiological information.
3. A qSOFA monitoring indicator for sepsis.
4. A Patient at Risk (PaR) system for medical staffs to focus on the management of patient at risk of deterioration.
5. To ensure that all healthcare professionals are communicating effectively, the ISBAR communication tool has been developed. ISBAR stands for Identify, Situation, Background, Assessment, and Response/Recommendations.
6. A model of interprofessional team communication based on social media, and the chat logs will be recorded in the Progress Note, becoming a part of the Electronic Medical Records (EMR).
7. The SDM (Shared Decision-Making) model is an approach whereby clinicians and patients share the best available evidence when faced with different therapies.
8. All core UI is based on social media, with LINE as the entrance point, and real-name users restricting information and ensuring data security.
The system will automatically update the patient’s seven physiological information every 10 minutes. The higher the score, the more serious it is. Moreover, all physiological information will be converted into visual charts for medical staff to quickly identify the patient’s current physiological state.
LINE User ID
The LINE real-name system uses the LINE UID, which is the unique user serial number generated by the random number of the LINE system.Every LINE user's account has a unique internal identification called a User ID.The format and purpose of User IDs and LINE IDs customized by LINE users are completely different.When developing Messaging API applications, whether to receive messages, send messages, or access other APIs, User IDs must be used to represent LINE users.The format of User ID is a 33-character alphanumeric string, such as U206d25c2ea6bd87c17655609a1c37cb8.
The feature of User ID is that each LINE user has a unique identification code for each company/organization on the LINE platform development account of each company/organization.That is, each Messaging API account under the same company/organization will use the same User ID to contact the same LINE user.
And the Messaging of different companies/organizations
API accounts must use different User IDs to contact the same LINE user.
This ensures that each company/organization cannot obtain or use the exclusive User ID of other companies/organizations, and protects the privacy and security of the company/organization and LINE users
LINE實名制是使用LINE UID這是LINE 系統亂數產生的使用者唯一序號,每一個LINE用戶帳號都有一個專屬的內部識別碼,稱為User ID。User ID與LINE用戶自訂的LINE ID的格式與用途完全不同。開發Messaging API應用程式時,無論是接受訊息、傳送訊息、或是存取其他API,皆必須使用User ID來代表LINE用戶。User ID的格式為33個字元的英數字字串,例如U206d25c2ea6bd87c17655609a1c37cb8。User ID的特色就是每一個LINE用戶在每一個公司/組織的LINE平台開發帳號都有該公司/組織專屬的識別碼,也就是相同公司/組織下的每個Messaging API帳號聯繫相同的LINE用戶會使用一樣的User ID,而不同公司/組織的Messaging
API帳號聯繫相同的LINE用戶就必須使用各自不同的User ID。如此確保每一個公司/組織都無法取得或使用其他公司/組織專屬的User ID,保障公司/組織與LINE用戶的隱私安全